ULCERATIVE COLITIS
What is ulcerative colitis?
Ulcerative colitis is inflammation of the colon, which is the lower part of the bowel (intestine) and digestive system. By the time food passes through six and a half metres of small intestine and reaches the colon, most of the food has been absorbed and only waste products are left. It is the job of the colon to absorb the excess water from the waste (as well as some fibre and potassium) and move the waste to the rectum. 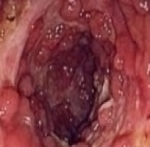 This becomes your bowel motion. When the bowel becomes inflamed, swelling and ulcers develop in the colon.
This becomes your bowel motion. When the bowel becomes inflamed, swelling and ulcers develop in the colon.
This is known as ulcerative colitis. It is a chronic condition. People with ulcerative colitis have a higher chance of getting cancer of the colon – more so if the disease begins before the age of 15 or continues for longer than 10 years.
What causes ulcerative colitis?
The exact cause of ulcerative colitis is unknown. It is thought to be a type of autoimmune disease. This means the tissue in the bowel becomes allergic to itself. Ulcerative colitis seems to occur more in some families but it is not clear whether it is due to hereditary or environmental factors. Ulcerative colitis may occur at any age, but it is most common in young adults in the 15–30 age group or later on, in the 50–70 age group. Women are affected more than men. Some foods can make symptoms worse but this is on an individual basis with no specific foods being common to all people. Some people believe that their symptoms are worse during periods of high stress but flare-ups are just as likely to occur after a bout of the flu. Most cases of ulcerative colitis are mild, but once symptoms are identified it is important to receive prompt medical attention because the condition can progress very quickly.
What are the symptoms?
The main symptoms are frequent attacks of bloody diarrhoea and pain in the lower abdomen (of varying intensity). This is interspersed with periods of no symptoms at all. Most often an attack begins slowly and with mild symptoms such as an increased urgency to have a bowel motion, mild lower abdominal cramps, and blood and mucus appearing in the bowel motions. Pus may be present. Ulcerative colitis may cause weight loss, fever, dry mouth, and sunken eyes, a fast heart beat, and pale skin. Loss of appetite, nausea and vomiting can occur. There may be some difficulty controlling bowel motions and it may feel that the bowel has not emptied properly. When you are examined by your doctor your bowel near your anus will most likely be inflamed.
Diagnosis
Blood tests will be taken and specimens of your bowel motions will be sent to the laboratory for examination to rule out an infectious cause of the colitis.
Your doctor will probably arrange a test on your lower bowel called a sigmoidoscopy. A narrow tube containing a camera and a light is passed through your anus into the lower bowel. This allows a specialist to look at the lining of your colon. Sometimes a small piece of tissue is removed (biopsy) so it can be examined more closely in a laboratory. Another procedure called a colonoscopy may also be carried out. This allows a higher part of your colon to be examined. In addition, a barium enema is sometimes necessary to see how far the inflammation has spread. A barium enema is an x-ray procedure which involves feeding a type of dye, barium, into the bowel through the back passage. A series of x-rays are then taken which show the outline of the inside of the bowel. These tests may be a bit uncomfortable but are not usually painful.


