CROHN'S DISEASE
What is Crohn’s disease?
Crohn's disease is a condition in which there is swelling, thickening and inflammation of one or more parts of the gastrointestinal tract from the mouth to the anus. Any part can be affected, but it is more common in the last part of the small bowel and colon. The normal function of the bowel is to absorb the food and liquid we consume and move the waste to the rectum – this becomes the bowel motion. If parts of the bowel become inflamed due to Crohn’s disease, normal absorption does not take place.
What causes Crohn's disease?
The cause is unknown. Heredity or environmental factors may play a part in the development – one in four people with Crohn’s disease have a relative with Crohn’s disease or ulcerative colitis. Various theories have been suggested. These include possible infection with agents such as bacteria, viruses, chlamydiae and, most recently, mycobacteria. Dietary factors (including chemicals and the low fibre diet consumed in modern developed countries) have also been implicated. None of these theories have been proved. Recent research into the heredity of Crohn’s disease has identified a human gene, called NOD2, and damage to this gene is believed to be associated with the disease in about 15% of those affected. While this discovery does not hold out the immediate prospect for a cure, it does mean that more certain diagnosis may become possible. It seems that this gene plays an important role in the interaction of the body’s immune system with gut bacteria.
What are the symptoms?
Symptoms depend on the location and extent of the inflammation. Chronic diarrhoea associated with abdominal pain, fever, anorexia, weight loss and a right lower abdominal pain and tenderness are the most common features. Sometimes the inflammation is so great that it blocks movement through the bowel. This can cause vomiting and/or constipation. The faeces may sometimes contain blood or appear pale and float. The area in and around the anus can also be affected by ulcers, abscesses or fistulas (small holes in the wall of the bowel or rectum). Children may not have prominent gastrointestinal symptoms but instead have unexplained joint or bone pain, fever, anaemia or stunted growth. When only the colon is affected, the symptoms may be indistinguishable from ulcerative colitis.
Diagnosis
Examination by your doctor and a blood test are the first steps in diagnosing Crohn’s disease. Definitive diagnosis is usually made by x-ray. A referral will then be made to a radiologist for further tests. These may include:
Barium meal or barium enema – Flavoured barium solution is swallowed (meal), or fed into the bowel through the anal canal (enema), and a series of x-rays are taken which show the outline of the inside of the bowel wall.
Colonoscopy – Colonoscopy involves the insertion of a narrow tube into the lower bowel through the anal canal. The tube contains a small camera with its own light source that allows the specialist to look at the lining of your colon. Sometimes a small piece of tissue is removed (biopsy) so it can be examined more closely in a laboratory.
Types of Crohn’s Disease
The symptoms and potential complications of Crohn’s disease differ, depending on what part of the GI tract is inflamed. That’s why it is important for you to know which part of your intestine is affected by Crohn’s disease. Your doctor also may refer to your illness by various names based on the main area involved.
The following are several types of Crohn’s disease:
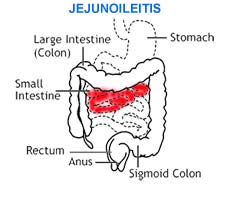 |
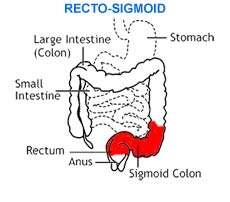 |
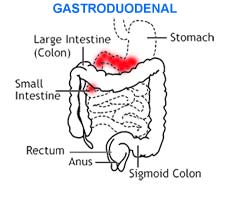 |
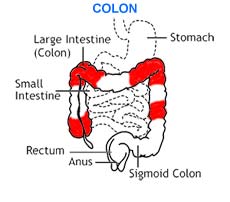 |
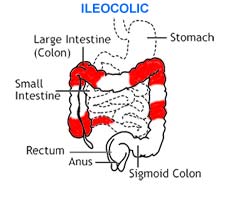 |
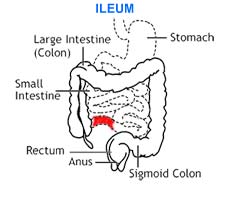 |
Surgery
Surgery is usually necessary when the bowel persistently becomes blocked or when there are abscesses or small holes in the bowel wall. Surgical removal of the part of the bowel that is badly affected may relieve symptoms indefinitely but it does not cure the disease. Recurrence rate after surgery, usually where the bowel has been joined, is 60 to 95%. Ultimately a further operation is required in nearly 50% of cases.
Surgery is not performed unless specific complications or failure of medical therapy make it necessary. When operations have been performed, however, most patients consider their quality of life has been improved.
Established chronic Crohn’s disease is characterised by lifelong recurrences. Growth retardation commonly results when the disease occurs during the developmental years. The disease rarely spreads without surgical manipulation of the bowel.
People with long-standing Crohn’s disease of the small intestine carry an increased risk of small bowel cancer, and those with Crohn’s colitis (Crohn’s disease that is only found in the colon) have a long term risk of colon cancer.


